Minimally Invasive Cardiac Procedures
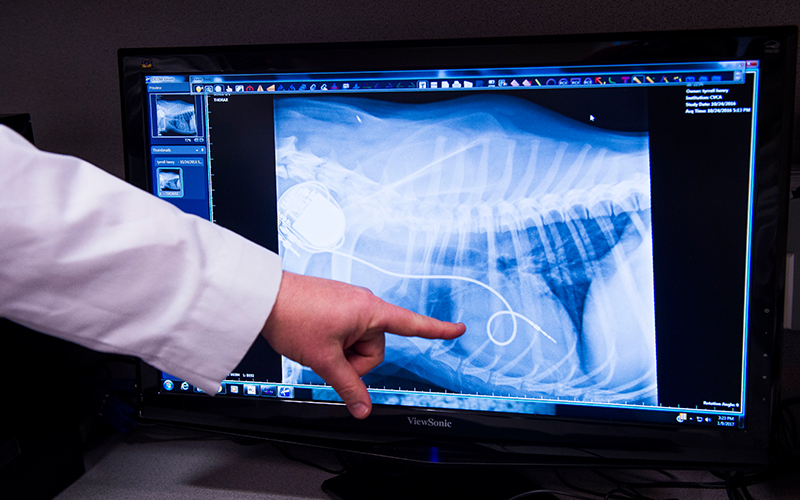
Minimally invasive cardiac procedures (sometimes called interventional procedures) are a category of treatments for certain heart conditions that allow the veterinary cardiologist to treat or correct the problem without invasive heart surgery.
These procedures include:
- balloon valvuloplasty
- pacemaker implantation
- catheter occlusions
- catheter ablation.
They are performed in a cardiac cath lab. Fluoroscopy (video X-rays) and echocardiography (ultrasound of the heart) provide imaging to help guide the procedure in the cath lab.
What happens during these procedures?
The animals are placed under anesthesia and are closely monitored. A catheter is placed into a vein or artery in either the groin or the neck providing access to the vessel. Then a thin guide wire is passed through the catheter into the vessel and is advanced under image guidance to the area of interest in or near the heart.
In most types of minimally invasive cardiac procedures, a long catheter is then passed over the guide wire. Contrast solution is injected through the catheter; this creates a roadmap (angiogram) that is viewed on the fluoroscopy unit. Once the catheter or guide wire is placed, the interventional device is passed into position. This is usually a balloon catheter (if the defect needs to be stretched out), an occluder or coil (if the defect needs to be plugged up) or an electrode (if an abnormal heart rhythm needs to be corrected).
What conditions are treated with these procedures?
The most common conditions treated this way are several congenital heart defects and some types of arrhythmias. A partial list of conditions treated by minimally invasive cardiac procedures includes:
- Pulmonic stenosis – a narrowing of the pulmonary artery.
- Aortic and sub-aortic stenosis – a narrowing of the aorta.
- Patent ductus arteriosis (PDA) – a shunt connecting the aorta and pulmonary artery.
- Ventricular septal defect (VSD) – a hole connecting the right and left ventricles.
- Atrial septal defect (ASD) – a hole connecting the right and left atria.
- Atrio-ventricular heart block – an abnormal rhythm producing a very slow heart rate.
- Re-entry tachycardia – an abnormal rhythm producing a very fast heart rate.
- Sick sinus syndrome – an abnormal rhythm producing an intermittently fast and slow heart rate.
In the near future, we may also be able to treat degenerative valve disease (the most common type of heart disease in dogs) via a minimally invasive method.
What are the signs and symptoms of heart disease?
The signs and symptoms vary depending on the underlying heart disease. The symptoms associated with the congenital heart diseases can include:
- Abnormal heart sounds (murmurs)
- Arrhythmias
- Weakness
- Collapse
- Labored breathing
- Heart failure.
The various arrhythmias treated with minimally invasive procedures are characterized by either very fast or slow heartbeats. The resulting symptoms include weakness, collapse, and syncope (fainting). In some cases, heart failure can develop which will lead to fluid accumulating in the chest and/or abdomen producing labored breathing.
How are these conditions diagnosed?
These various conditions are diagnosed based on a review of the clinical signs and history followed by a physical examination, and a combination of tests including chest radiographs (X-rays), echocardiogram (ultrasound imaging of the heart) and ECG (electrocardiogram). Once the initial testing is performed, a cardiac catheterization may be performed to record pressures across a narrowing or measure the volume of blood being shunted across a defect. In some cases, an angiogram will be needed to determine what size device will be needed to close a defect. The angiogram will also provide the road map to follow to position the device in the proper location.
Treatment and Aftercare
Once all of the diagnostics and are completed the intervention (treatment) is performed.
- Stenosis (pulmonic and aortic) – a balloon catheter is positioned across the stenotic (narrowed) valve and is inflated with a mixture of saline and contrast material under high pressure. The image is viewed on the fluoroscopy screen and the inflation is repeated multiple times until the stenosis is stretched out. This procedure is called a balloon valvuloplasty.
- Shunts (PDA, VSD, ASD) – a guiding catheter is placed across the defect with the aid of fluoroscopic guidance and sometimes ultrasound guidance. The occluding device (usually an Amplatzer occluder) is pushed through the catheter into position across the defect plugging the shunt. This procedure is called a catheter occlusion.
- Arrhythmias (heart block, sick sinus syndrome) – An electrical lead wire is passed down the jugular vein in the neck and attached into the bottom of the right ventricle in the heart. The other end of the lead wire is attached to a pulse generator (e.g. pacemaker) and buried under the skin in the neck area. This procedure is called a pacemaker implantation.
- Re-entry arrhythmias (reentry tachycardia) – Special electrodes are passed through a catheter into the atria (the two top chambers of the heart) and used to map out the source of the arrhythmia. This procedure is called an EP study. Once the location is identified, another specialized catheter is placed in position and a pulse of focused high energy is transmitted through the catheter to the re-entry site. This destroys the re-entry pathway and returns the heart rhythm to normal. This procedure is called a catheter ablation.
After these procedures are completed, the patients are monitored closely overnight and usually discharged the following day.
Prognosis
The prognosis for these different diseases after the procedures have been performed is generally very good but may vary on a case to case basis. The patient’s status should be monitored at regular intervals by the Veterinary Cardiologist to ensure the best possible outcome.
Articles by Specialty
- Cardiology (19)
- Large Animal Internal Medicine (23)
- Neurology (17)
- Oncology (22)
- Small Animal Internal Medicine (29)
Articles by Animal
- Cats (35)
- Dogs (52)
- Farm Animals (5)
- Horses (12)
